Orofacial Pain Phoenix, AZ
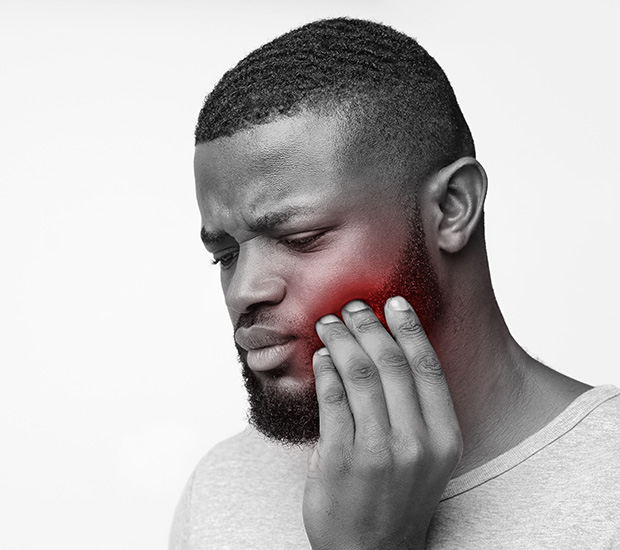
Orofacial pain describes any pain or discomfort in the head, neck, face, jaw, or mouth. With varying levels of sensitivity, the causes of orofacial pain can vary widely. This is why patients need a professional diagnosis from a dental professional so they receive the most effective treatment to meet their needs.
At Sundance Dental Care, we treat patients in Phoenix and the surrounding area to help them achieve lasting relief with professional solutions that address the source of their orofacial pain. Our team will examine your unique case and discuss treatment options. Call us at (623) 687-2993 to schedule an appointment today.
What is orofacial pain?
According to the scientific journal, Diagnostics, Orofacial pain or OFP represents “one of the most common health problems that negatively affects the activities of daily living.” OFP can describe pain and dysfunction symptoms in the head, mouth, face, jaws, or neck. These symptoms can range from mild to severe, and may include more than just dental and jaw pain. Headaches, neck and ear pain, burning sensations in the face, ringing in the ears (tinnitus), dizziness, abnormal itching, and incoordination of the head, neck, and facial muscles can all be symptoms of oral facial pain. This pain not only impacts oral function but also contributes to difficulty sleeping and significantly impacts quality of life.
“OFP can describe pain and dysfunction symptoms in the head, mouth, face, jaws, or neck.”
OFP can describe pain and dysfunction symptoms in the head, mouth, face, jaws, or neck.
Multiple causes and risk factors can lead to OFP, and in some cases, more than one factor contributes to the problem. Common causes and risk factors include the following:
Dental issues
Toothache, gum disease, abscesses, tooth decay, and other related gum and dental issues are generally considered the most common causes of orofacial pain. Risk factors for these issues can include a genetic predisposition, but typically involve poor dental hygiene and untreated gum and dental problems.
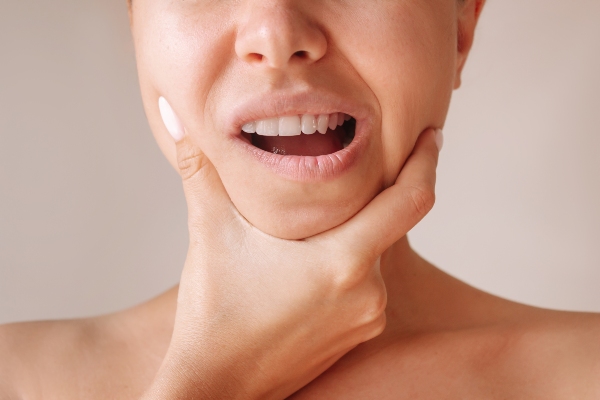
Temporomandibular Joint Disorder (TMD)
As the name suggests, TMD is a condition affecting the temporomandibular joint (TMJ) and associated muscles, and it is generally considered the second most common cause of OFP. Risk factors contributing to TDM include orthodontic issues, trauma, arthritis, and even stress-related dental habits such as teeth grinding, also known as bruxism.
Nerve damage
Nerve compression, injury, or other types of damage can lead to chronic orofacial pain. Conditions like trigeminal neuralgia, involving sudden and intense bouts of facial pain, can be the result of nerve damage or irritation. The condition is more common in females, and other risk factors include hypertension, smoking, and age.
Muscle stress and strain
Chronic stress can lead to muscle tension in the neck and head and worsen orofacial pain. Poor posture is a leading contributing factor.
OFP trauma or injuries to the jaw or face, especially those not treated correctly. Additional risk factors for orofacial pain can include genetic factors, certain infections, and mental health disorders such as anxiety and depression.
“As the name suggests, TMD is a condition affecting the temporomandibular joint (TMJ) and associated muscles, and it is generally considered the second most common cause of OFP.”
Benefits of treatment from a general dentist
Orofacial pain, especially that stemming from TMD, can affect daily life in ways beyond the jaw. Receiving orofacial pain treatment from a general dentist keeps care practical and coordinated, especially when symptoms overlap with tooth wear, gum irritation, or bite changes. They can also help rule out dental causes of pain that mimic TMJ symptoms, such as cracked teeth, cavities, or inflammation around old restorations.
One key benefit is receiving a comprehensive evaluation in a single setting. The dentist can assess bite alignment, enamel wear patterns, muscle tenderness, and joint function, and also check the teeth and gums for related issues. That broader view helps connect symptoms to likely triggers, such as clenching, grinding, or a bite imbalance that places strain on the jaw muscles. When the dentist evaluates both oral health and joint function together, treatment recommendations tend to be more personalized.
Another benefit is access to conservative, comfort-focused options. Many cases improve with non-surgical care, such as bite adjustments, night guards, anti-inflammatory guidance, and habit coaching, designed to reduce strain on the jaw. A general dentist can also recommend supportive strategies at home, including heat and cold therapy, soft-food periods during flare-ups, and posture or sleep-position tips to reduce muscle tension. This conservative approach supports symptom relief without jumping to invasive interventions.
A general dentist also supports continuity of care over time. Since orofacial pain symptoms often fluctuate, depending on the root cause, follow-up visits help track patterns and fine-tune treatment based on real-life response. If a nightguard needs adjustment, bite contacts change, or a new trigger develops, the dentist can update care quickly. Ongoing monitoring also helps protect teeth from damage related to grinding, including chips, cracks, and premature wear.
Finally, coordinated referrals are easier to arrange when needed. If symptoms suggest a more complex TMJ disorder, airway concerns, or a condition that warrants specialty evaluation, a general dentist can refer patients to the appropriate specialist while continuing to manage oral health and protective care. This team-based approach helps patients avoid treatment gaps and keeps the focus on both comfort and long-term function.
“Receiving orofacial pain treatment from a general dentist keeps care practical and coordinated, especially when symptoms overlap with tooth wear, gum irritation, or bite changes.”
Check out what others are saying about our general-dentist services on Yelp: Orofacial Pain in Phoenix, AZ
Orofacial pain treatment
Our general dentist provides customized treatment plans to address the specific cause of the pain. Treatment usually involves a combination of medication, physical therapy, dental work, and other interventions. Common treatments include:
- Medication. Pain medications and muscle relaxers are often prescribed along with medications for nerve pain, such as gabapentin.
- Dental treatments.Can include anything from fillings and root canals to extractions and night guards for teeth grinding.
- Physical therapy.Includes jaw exercises, massage, and manipulation for those with TMD and may include posture guidance.
- Botox. Most commonly associated with cosmetic improvements, these injections can help treat TMD and other sources of OFP.
- Surgical interventionIf less invasive treatments have not produced the necessary improvement, the dentist may recommend surgery.
The goal is to relieve pain and other symptoms, repair any damage, and address the root cause of the problem in order to produce lasting relief.
“Treatment usually involves a combination of medication, physical therapy, dental work, and other interventions.”
Questions Answered on This Page
Q. What are the causes and risk factors for orofacial pain?
Q. What are the benefits of seeing a general dentist for orofacial pain?
Follow-up care
The key to ensuring this lasting relief is follow-up and ongoing care, involving a combination of continued monitoring, treatment, and lifestyle modifications. Each patient's follow-up plan will be different, but it will likely involve regular check-ins to ensure treatments remain effective and to determine whether adjustments are necessary. Continued commitment to regular dental checkups is also crucial, especially for patients with a history of teeth grinding, TMJ, or other dental issues.
Self-care is essential to ensure lasting relief. Thus, patients need to continue healthy habits and routines that reduce the risk of recurring orofacial pain. Healthy lifestyle practices include stress management, relaxation techniques, posture exercises, proper nutrition, and dental hygiene. While these should not replace professional treatment, they are effective at helping patients maintain lasting relief.
“Thus, patients need to continue healthy habits and routines that reduce the risk of recurring orofacial pain.”
Frequently Asked Questions (FAQs) About Orofacial Pain
Q. How do I know I am struggling with orofacial pain?
A. While conditions that cause orofacial pain can be similar, a licensed professional can identify the source and diagnose the condition. With a proper diagnosis, patients can receive the treatment they need. These conditions, including temporomandibular joint (TMJ) disorders and dental problems like tooth decay or gum disease, are among the leading causes of OFP. Muscle tension in the face and jaw, often due to stress, can also lead to severe pain and discomfort.
Q. When do I need to see a general dentist?
A. It is highly beneficial to schedule an appointment if the pain persists for several days or impairs daily activities like eating or speaking. We can diagnose complex pain conditions and offer a personalized treatment plan tailored to a patient’s unique needs. There is no reason to continue masking the pain or symptoms with OTC medication. Addressing the pain at the source will lead to lasting relief.
Q. Is there a cure for orofacial pain?
A. While many cases of orofacial pain can be treated effectively, leading to a meaningful reduction or elimination of symptoms, the success of the treatment relies on pinpointing the underlying cause. If the the treatment does not address the underlying cause, then the symptoms will return over time. In fact, conditions such as chronic nerve pain or TMJ disorders require ongoing management. Fortunately, our team can help patients with OFP achieve long-term relief with the right treatment plan.
Q. Can I manage orofacial pain at home?
A. Even though there might be several home remedies that help to alleviate mild orofacial pain, more severe instances require professional care. Along with that, at-home remedies will only provide temporary relief. With professional treatment, patients can achieve lasting relief and learn effective management techniques to avoid recurring symptoms in the future.
Q. Can stress contribute to orofacial pain?
A. Yes. In many cases, stress can either cause or exacerbate orofacial pain. Stress often leads to behaviors that strain the muscles and joints of the face, such as teeth grinding or jaw clenching. While there are techniques to help manage orofacial pain from stress, a licensed dental professional can address the true source of the pain and recommend how to achieve lasting relief.
Getting to the bottom of your orofacial pain
Orofacial pain should not interfere with your daily life. Contact Sundance Dental Care at (623) 687-2993 for more information on solutions to orofacial pain. Our team provides diagnosis and treatment in Phoenix and the surrounding communities.
If you live in the Phoenix area, call 623-687-2993 for an appointment in our Phoenix office.
Helpful Related Links
- American Dental Association (ADA). Glossary of Dental Clinical Terms. 2026
- American Academy of Cosmetic Dentistry® (AACD). Home Page. 2026
- WebMD. WebMD’s Oral Care Guide. 2026
About our business, license, and website security
- Sundance Dental Care was established in 2011.
- We accept the following payment methods: American Express, Cash, Check, Discover, MasterCard, and Visa
- We serve patients from the following counties: Maricopa County
- We serve patients from the following cities: Phoenix, Tolleson, Avondale, Goodyear, Glendale, Litchfield Park, Laveen Village, Buckeye, Estrella and Peoria
- AZ (License #D07361). View License Information and Specifics
- National Provider Identifier Database (1912067596). View NPI Registry Information
- Norton Safe Web. View Details
- Trend Micro Site Safety Center. View Details
Back to top of Orofacial Pain